Endodontics
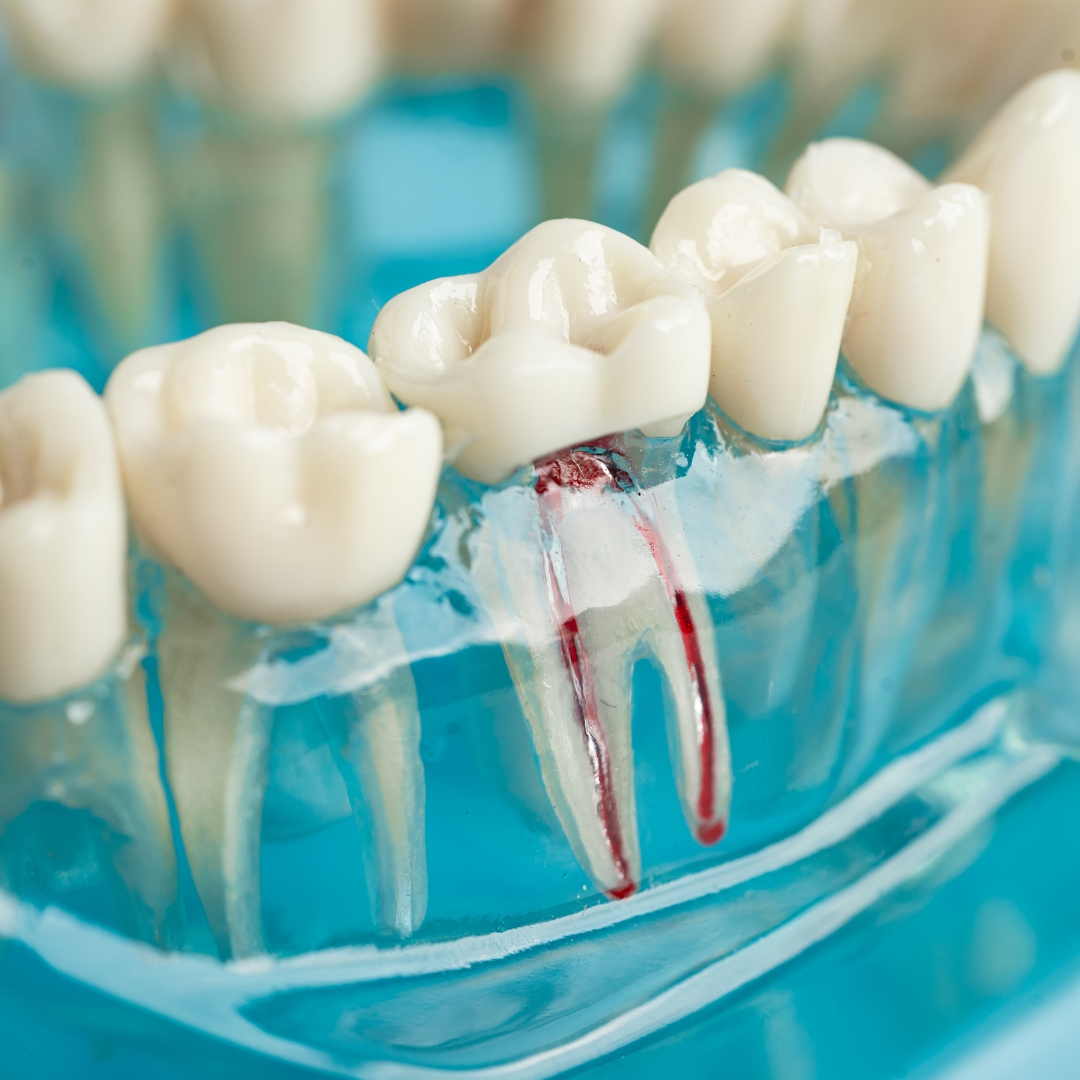
If you require endodontics, Joanna Man is here to help you.
There are three different types of treatments and procedures:-
- Endodontic therapy aka root canal treatment
- Endodontic retreatment
- Endodontic surgery
Endodontic therapy (aka root canal treatment)
What is the difference between endodontics and root canal?
The term 'root canal' when meaning endodontic therapy is, in fact, wrong. Root canals are part of a tooth, the hollows within a tooth where the nerve tissue, blood vessels, and some other cells are located. Root canal is a place in a tooth, while endodontic therapy is a dental procedure. However, the term 'root canal' has become widely used with the meaning of endodontic therapy.
What is endodontic therapy?
Endodontics (from the Greek roots endo- "inside" and odont- "tooth") is the dental specialty concerned with the study and treatment of the dental pulp.
To understand endodontic treatment, it helps to know something about the anatomy of the tooth. Inside the tooth, under the white enamel and a hard layer called the dentin, is a soft tissue called the pulp. The pulp contains blood vessels, nerves, and connective tissue and creates the surrounding hard tissues of the tooth during development.
The pulp extends from the crown of the tooth to the tip of the roots where it connects to the tissues surrounding the root. The pulp is important during a tooth's growth and development.
However, once a tooth is fully mature it can survive without the pulp, because the tooth continues to be nourished by the tissues surrounding it.
When is endodontic treatment necessary?
Endodontic treatment is necessary when the pulp, the soft tissue inside the root canal, becomes inflamed or infected. The inflammation or infection can have a variety of causes:
- deep decay
- repeated dental procedures on the tooth
- a crack or chip in the tooth
- dental trauma
In addition, an injury to a tooth may cause pulp damage even if the tooth has no visible chips or cracks.
If pulp inflammation or infection is left untreated, it can cause pain or lead to an abscess.

Joanna “One of the most common things people say to me is “I’d rather give birth than have root canal treatment”.
Another is “Root canal – that must be agony”. That’s a lot of negative connotations. And that’s probably why half the population don’t have a routine dental appointment; they only come in when something’s hurting and they’ve no other choice.
But I get to know my patients really well. I form quite a bond with them. Quite often I don’t talk about their teeth at all for the first five minutes as we’re busy catching up on all their family or job news. It’s all very relaxed.”
Signs that endodontic treatment might be necessary
Signs to look for include pain, prolonged sensitivity to heat or cold, tenderness to touch and when chewing, discoloration of the tooth, and swelling, drainage and tenderness in the lymph nodes as well as nearby bone and gum tissues. Sometimes, however, there are no symptoms.
How endodontic treatment saves the tooth
The dentist removes the inflamed or infected pulp, carefully cleans and shapes the inside of the root canal, then fills and seals the space. Afterwards, you will return to your dentist, who will place a crown or other restoration on the tooth to protect and restore it to full function.
After restoration, the tooth continues to function like any other tooth.
The endodontic procedure
Endodontic treatment can often be performed in one or two or more visits and involves the following steps:
- The dentist examines and x-rays the tooth, then administers local anaesthetic.
- After the tooth is numb, the dentist places a small protective sheet called a “rubber dam” over the area to isolate the tooth and keep it clean and free of saliva during the procedure.
- The dentist makes an opening in the crown of the tooth. Very small instruments are used to clean the pulp from the pulp chamber and root canals and to shape the space for filling.
- After the space is cleaned and shaped, the dentist fills the root canals with a rubberlike material called gutta-percha. The gutta-percha is placed with a cement to ensure complete sealing of the root canals.
- In most cases, a temporary filling is placed to close the opening. The temporary filling will be removed by your dentist before the tooth is restored.
- After the final visit with the dentist, the patient must return to have a crown or other restoration placed on the tooth to protect and restore it to full function. If the tooth lacks sufficient structure to hold the restoration in place, the dentist may place a post inside the tooth. The dentist will give more details about the specific restoration planned for the tooth.
Will the patient feel pain during the procedure?
Many endodontic procedures are performed to relieve the pain of toothaches caused by pulp inflammation or infection. With modern techniques and anaesthetics, most patients report that they are comfortable during the procedure.
For the first few days after the treatment, the patient's tooth may feel sensitive, especially if there was pain or infection before the procedure. This discomfort can be relieved with over-the-counter or prescription medications. The patient should follow the dentist's instructions carefully.
The tooth may continue to feel slightly different from the other teeth for some time after the endodontic treatment is completed. However, if there is severe pain or pressure or pain that lasts more than a few days, call the dentist.
Local anaesthetic via the wand
The wand is a computer-controlled dental injection device for giving local anaesthetic. The flow rate of the local anaesthetic is controlled by the computer, which ensures that it is slow, steady and therefore comfortable.
The precise control of the anaesthetic flow rate and pressure reliably produces a comfortable injection, even in areas of the mouth where an injection may be slightly more difficult for the dentist such as the palate. The wand reduces your anxiety, allows faster numbing onset and sensation recovery, giving predictable deep anaesthesia.
Are any teeth not suitable for endodontic treatment?
Most teeth can be treated. Occasionally, a tooth can't be saved because the root canals are not accessible, the root is severely fractured, the tooth doesn't have adequate bone support, or the tooth cannot be restored.
However, advances in endodontics are making it possible to save teeth that even a few years ago would have been lost. When endodontic treatment is not effective, endodontic surgery may be able to save the tooth.
Will the tooth need any special care or additional treatment after endodontic treatment?
The patient should not chew or bite on the treated tooth until they have had it restored by their dentist. The unrestored tooth is susceptible to fracture, so they should see their dentist for a full restoration as soon as possible.
The patient should practice good oral hygiene, including brushing, flossing, and regular examinations and cleaning.
How long will the treated tooth last?
Most endodontically treated teeth last as long as other natural teeth. In a few cases, a tooth that has undergone endodontic treatment does not heal or the pain continues.
Occasionally, the tooth may become painful or diseased months or even years after successful treatment. Often when this occurs, re-doing the endodontic procedure can save the tooth.
What causes an endodontically treated tooth to need additional treatment?
New trauma, deep decay, or a loose, cracked or broken filling can cause new infection in your tooth. In some cases, the dentist may discover additional very narrow or curved canals that could not be treated during the initial procedure.
Endodontic retreatment
With proper care, even teeth that have had root canal treatment can last a lifetime.
But sometimes, a tooth that has been treated doesn't heal properly and can become painful or diseased months or even years after treatment.
If a tooth failed to heal or develops new problems, the patient has a second chance. An additional procedure may be able to support healing and save the tooth. If the patient has pain or discomfort in a previously treated tooth, they should talk to the dentist about retreatment.
Why might endodontic retreatment be necessary?
As occasionally happens with any dental or medical procedure, a tooth may not heal as expected after initial treatment for a variety of reasons:
- Narrow or curved canals were not treated during the initial procedure
- Complicated canal anatomy went undetected in the first procedure
- The placement of the crown or other restoration was delayed following the endodontic treatment
- The restoration did not prevent salivary contamination to the inside of the tooth.
In other cases, a new problem can jeopardise a tooth that was successfully treated. For example:
- New decay can expose the root canal filling material to bacteria, causing a new infection in the tooth
- A loose, cracked or broken crown or filling can expose the tooth to new infection
- A tooth sustains a fracture.
What will happen during retreatment?
First, the dentist will discuss the patient's treatment options. If the patient and dentist choose retreatment, the dentist will re-open their tooth to gain access to the root canal filling material. In many cases, complex restorative materials—crown, post and core material—must be disassembled and removed.
After removing the canal filling, the dentist can clean the canals and carefully examine the inside of the tooth using magnification and illumination, searching for any additional canals or unusual anatomy that requires treatment.
After cleaning the canals, the dentist will fill and seal the canals and place a temporary filling in the tooth. If the canals are unusually narrow or blocked, the dentist may recommend endodontic surgery, which involves making an incision to allow the other end of the root to be sealed.
After the dentist completes retreatment, the patient will need to return to their dentist as soon as possible to have a new crown or other restoration placed on the tooth to protect and restore it to its full function.
Is retreatment the best choice?
Whenever possible, it is best to save the natural tooth. Retreated teeth can function well for years, even for a lifetime.
Advances in technology are constantly changing the way root canal treatment is performed, so the dentist may use new techniques that were not available when the patient had their first procedure. The dentist may be able to resolve the problem with retreatment.
As with any dental or medical procedure, there are no guarantees. The dentist will discuss the options and the chances of success before beginning retreatment.
What are the alternatives to retreatment?
If non-surgical retreatment is not an option, then endodontic surgery should be considered. This surgery involves making an incision to allow access to the tip of the root.
Endodontic surgery may also be recommended in conjunction with retreatment or as an alternative. The dentist will discuss the options and recommend appropriate treatment.
Endodontic surgery
Very occasionally, a non-surgical root canal procedure alone cannot save the tooth, in this case the dentist can offer to provide surgery, although in some cases he may recommend a referral elsewhere.
What is endodontic surgery used for?
Endodontic surgery can be used to locate small fractures or hidden canals that weren't detected on x-rays or during previous treatment.
Surgery may also be needed to remove calcium deposits in root canals, or to treat damaged root surfaces or the surrounding bone of the tooth.
There are many surgical procedures that can be performed to save a tooth. The most common is called an apicectomy, or root-end resection, which is occasionally needed when inflammation or infection persists in the bony area around the end of the tooth after a root canal procedure.
What is an apicectomy?
In this procedure, the dentist opens the gum tissue near the tooth to see the underlying bone and to remove any inflamed tissue. The very end of the root is also removed.
A small biocompatible filling is placed in the root to seal the end of the root canal, and a few stitches or sutures are placed in the gingiva to help the tissue heal properly.
Over a period of months, the bone usually heals around the end of the resected root. However, dependent upon the size of the initial lesion it can sometimes take up to a year. In some cases recurrence of swelling can occur and may require further surgery or extraction of the tooth.
What are the other types of endodontic surgery?
Other surgeries the dentist might perform include dividing a tooth in half, repairing an injured root, or even removing one or more roots.
The dentist will be happy to discuss the specific type of surgery the tooth requires. These procedures are designed to help save the tooth.
Will the procedure hurt?
Local anaesthetics make the procedure comfortable. Of course, the patient may feel some discomfort or experience slight swelling while the incision heals. This is normal for any surgical procedure.
The dentist will recommend appropriate pain medication to alleviate any discomfort and will give the patient specific post-operative instructions to follow. If you have questions after the procedure, or if you have pain that does not respond to medication, you should call the dentist.
Can the I drive myself home?
Often yes, but you should ask the dentist before the appointment so that you can make transportation arrangements if necessary.
When can I return to my normal activities?
Most patients return to work or other routine activities the next day. The dentist will be happy to discuss expected recovery time with you.
How does I know if the surgery will be successful?
The dentist is suggesting endodontic surgery because they believe it is the best option for saving the natural tooth. Of course, there are no guarantees with any surgical procedure. The dentist will discuss the chances for success so that you can make an informed decision.
What are the alternatives to endodontic surgery?
Often, the only alternative to surgery is extraction of the tooth. The extracted tooth can then be replaced with an implant, bridge, or removable partial denture to restore chewing function and to prevent adjacent teeth from shifting or opposing teeth from over erupting.
Because these alternatives require surgery or dental procedures on adjacent healthy teeth, endodontic surgery is usually the most biologic and cost-effective option for maintaining oral health.
Endodontics costs
Full details of all pricing and our 0% finance deal are available on our treatment costs page.


